To some, that scene reveals a virus that spreads through a room’s air like a phantom, lingering there and infecting those nearby. That makes the case for mandatory masks in crowded areas clear.
To other scientists and health leaders, it does not show that at all.
There is no strong evidence airborne spread is a major transmission route for the virus, they say.
Two of the most-senior infection-control experts advising the federal government belong to the latter group.
There are of course other factors at play. Up until now, Australia has not confronted the high levels of community transmission that make some experts think masks might be useful.

Customers wait outside the Perth Apple Store wearing masks on May 8.
But that fundamental disagreement goes a long way to explaining why Australia has remained reluctant to enforce compulsory mask-wearing even as more and more US states make face-coverings mandatory.
That started to change on Friday, as mounting community spread – and a significant new piece of evidence – encouraged the Victorian government to call on the community to wear masks in public.
Dogmas don’t die easy
When it comes to masks, experts agree on most things.
If you cough or sneeze, wearing a mask will help prevent you spreading a virus onto others. If you cannot socially distance and you’re in an area of high transmission, a face-covering is a good idea.
What many experts do disagree on is this: how far can COVID-19 travel through the air?

How far can a sneeze spread?
Respiratory viruses like COVID-19 spread through droplets – the tiny particles of virus-containing saliva or mucus we spray when we cough and sneeze. If infected droplets land on a person’s mouth, nose, or eye, the virus can gain entry into the body. If enough virus gets in, we can get sick.
That’s why the Australian government advises people to keep 1.5 metres away from each other.
The theory is, at that distance, all the big, heavy and highly infectious droplets from a cough or sneeze will drop to the ground before they can reach you.
That’s why social distancing and hand washing (to kill any droplets you may have on your hands) are health authorities’ front-line weapons, rather than masks.
But the belief that most virus-carrying droplets will fall out of the air over 1.5 metres is based on aging evidence that now looks increasingly shaky.
In the 1930s and 40s scientists tried to get an idea of how viruses spread by having people cough onto plates.
They then studied the size of the droplets under a microscope. Most of the droplets – about 95 per cent – were found to be too big to spread further than 1.5 metres.
But the tests they used were not sensitive enough to pick up tiny particles.
More recent studies have found the vast majority of particles generated are actually much more tiny than previously thought and can hang in the air for some time.
And these tiny particles are exiting our mouth all the time to waft about the room.
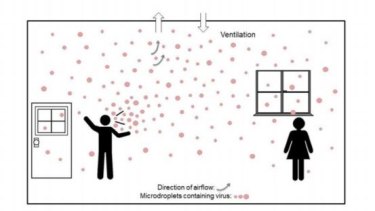
Credit:Oxford University Press
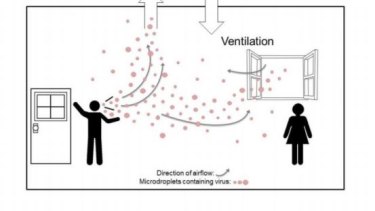
This diagram, from a paper by Professor Morawska, shows how a virus can spread through a poorly-ventilated room.Credit:Oxford University Press
Yet the 1.5 metre rule has become “dogma” and held up the push for masks, said Director of the WHO Collaborating Centre for Air Quality at the Queensland University of Technology Professor Lidia Morawska.
“If it’s not accepted the virus can be transmitted through the airborne route, you don’t need to wear a mask,” she said. “Dogmas don’t die easy.”
A simple meal
Let’s return, for a moment, to the restaurant in China.
One person infected with COVID-19 enters. Six leave.
Yet security camera footage reviewed later by scientists show the infected patient never coughed or sneezed on any of the people who fell sick – never had direct contact with any of them.
For Professor Morawska, that is clear evidence COVID-19 can spread indirectly and over long distances.
Two of Australia’s key infection control experts disagree.
Professor Lyn Gilbert is chair of the federal government’s Infection Control Expert Group, an influential body that advises the states’ chief health officers.
Associate Professor Philip Russo is deputy-chair, and president of the Australasian College for Infection Prevention and Control.
Speaking in their personal capacity as researchers, both told The Age and the Sydney Morning Herald they did not believe there was strong evidence airborne spread was a major transmission route for COVID-19.
“Wearing a mask is not as simple a solution that some people make out – and is unlikely to be effective on its own, irrespective of whether transmission is predominantly by droplets or sometime airborne,” said Professor Gilbert.
COVID-19 is spread by direct contact – being coughed or sneezed on. “If you’re that close to someone, you’ll get droplets on the other parts of your face. Even if you’re wearing a mask,” Dr Russo said. Most transmission happens in households, not in public spaces, he said.
Airborne spread “is not a major source of infection,” he said.
What about the Chinese restaurant? Professor Gilbert argued that was most likely direct spread, not airborne transmission – and at any rate, people cannot practically wear masks in restaurants.
“There may not be direct contact between people, but they are close together in small, crowded spaces,” she said. “That’s exactly the space where these small particles don’t have to hang in the air for very long to get to someone else.”
It is not clear the tiny droplets Professor Morawska worries about are big enough to contain enough virus to cause an infection.
Further, if COVID-19 really was airborne, it would behave more like measles – where every sick child infects about 12 to 18 others on average, said Dr Russo. COVID-19’s reproduction number hovers closer to 2 than 20.
“People who get the virus are those that have close contact. If this was a true airborne infection like tuberculosis or measles, that would come out in the epidemiology,” said Dr Russo.
“And the inappropriate wearing of masks can be more dangerous. You can end up touching the mask a lot, touching the face a lot, and end up contaminating yourself that way.”
Do masks work?
Setting aside how long COVID hangs in the air, the evidence for how well masks actually work to stop the spread of infection is more contested than you might think.
In part, that’s because there is no high quality direct evidence that shows asking the general public to wear masks prevents COVID-19, as the World Health Organisation says (the organisation, nevertheless, recommends masks).
One way to prove masks prevent the spread of COVID-19 is to run a randomised controlled trial. We don’t have one for COVID-19 yet.
That leaves us with randomised controlled trials of mask wearing to prevent the spread of the flu, which tend to show positive if modest results, and observational studies.
These studies look at virus transmission in groups of people who claim to wear masks all the time.
They can provide evidence only of a link, not an actual effect.
A major review of observational studies, published in the Lancet on June 1, found wearing a mask in the community reduced the risk of spreading COVID-19 by 69 per cent – a huge drop.
That paper has led many experts, as well as the Australian Medical Association, to back calls for mask-wearing in Melbourne.
“The effectiveness of masks reducing transmission is now really clear,” says Burnet Institute epidemiologist Professor Michael Toole.
“We hear that wearing a mask will make you stop washing your hands or forget to keep your distance from others – there is no science to support this. In fact, the science shows the opposite – that masks protect,” says head of biosecurity at the Kirby Institute Professor Raina MacIntyre.
It was also enough to swing Victorian Chief Health Officer Brett Sutton, who on Friday told media that study had provided the strong evidence he needed to make the call on asking Melburnians to wear masks in public.
Not everyone agrees.
“That Lancet study is seriously flawed,” said director of the Institute for Evidence Based Health Care at Bond University Professor Paul Glasziou.
“It’s all based on observational evidence. And they did not adjust for the confounding. Mask wearers are known to be worried people who do the appropriate behaviours: they socially distance, they worry more.”
He and a team of academics from Bond University reviewed 14 randomised controlled trials of masks. In a study that has not yet been peer reviewed or published, they found there was weak evidence masks reduced the risk of catching a flu-like illness.
One problem, Professor Glasziou said, is that even if people were educated on how to wear masks they typically did not wear them correctly or often enough. Masks also do not protect the eyes from droplets.
And as the WHO points out, studies have suggested wearing a mask can encourage people to regularly fiddle with it, potentially contaminating it, and may even create a false sense of security which may cause them to drop their guard.
“I’m not for or against masks,” Professor Glasziou said. “But if you think it is the magic ingredient that is going to stop the pandemic, I think you are fooling yourself.”
Get our Morning & Evening Edition newsletters
Liam is The Age and Sydney Morning Herald’s science reporter
Most Viewed in National
Loading











